Canada’s already undermanned and overstretched frontline healthcare workers fighting to stop the spread of COVID-19 need better physical and mental health protection support to endure what is likely to be a prolonged battle with the pandemic, says the Canadian Association of Emergency Physicians.
Dr. Rod Lim, who chairs the association’s wellness committee, said the physical and psychological health and safety of emergency department staff at Canadian hospitals is vital to the national interest.
Gearing up for ‘a very long period of immense stress’
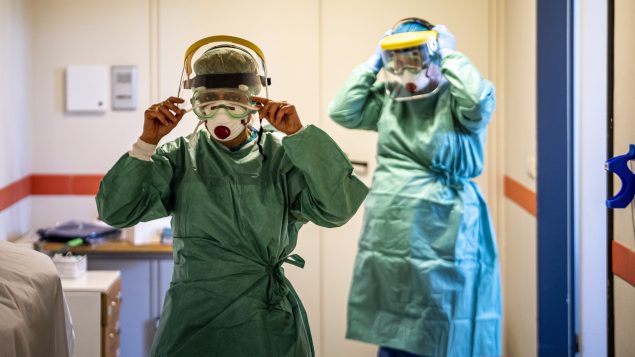
Nurses put on protective gear in a ward designated for new patents infected with the coronavirus in a hospital in Budapest, Hungary, Monday, March 16, 2020. Veterans from the frontlines of infectious disease see three potential challenges looming in the care of Canada’s sickest COVID-19 patients: intensive care space, surplus ventilators and keeping specialized staff healthy. (Zsolt Szigetvary/THE CANADIAN PRESS/MTI via AP)
The association has highlighted four critical areas to support frontline health professionals as they gear up for what will probably be “a very long period of immense stress,” said Lim, who’s also the medical director and section-chief of the Paediatric Emergency Department at the Children’s Hospital at London Health Sciences Centre.
These include protecting the health and safety of emergency department staff; optimizing human resource management; ensuring access to counselling and emotional support during the pandemic and in its aftermath; and developing a single centralized, authoritative source for the dissemination of information about the pandemic.
“Depending on the area of the country, we’re mostly in a preparation phase at this point but already we’re facing challenges in adaptation with new information, threats to supply of personal protective equipment,” said Lim.
“We are constantly faced with conflicting information. Depending on the source of information, information is rapidly changing due to the evolution of COVID-19.”
These challenges present profound difficulties for frontline medical staff, Lim said.
“We have to navigate this information and adjust almost on the hourly to daily basis,” he added.
Dealing with anxiety and fear

Members of the public wait to be tested at a COVID-19 assessment centre located at Michael Garron Hospital, in Toronto. (Evan Mitsui/CBC)
Frontline medical workers have to deal with anxiety and fear as they worry about their own health, the health of their families and their patients, Lim said.
“The breadth of the potential ramification of this pandemic on every aspect of our life is not lost on us,” Lim said.
There has to be a serious discussion about protecting vulnerable medical workers: those who are older or have some pre-existing medical conditions that put them at particular risk, Lim said.
The Canadian health care system already faces a projected shortage of 1,100 emergency department physicians, Lim said.
“People will rise to the occasion, but we cannot be blind to the cost,” Lim said. “Emergency medicine doctors across the world – and Canada is no exception – have already faced tremendous strain prior to the pandemic.”
Offering mental health support during and after the pandemic

Health workers demonstrate how to put on protective clothing during a tour of a COVID-19 evaluation clinic in Montreal on Tuesday.(Graham Hughes/Canadian Press)
Emergency medicine is already one of the highest risk professions for burnout in Canada, Lim said.
“You can’t believe that an unhealthy workforce, under a lot of strain, faced with an immense anxiety and threat, would not have a lasting toll,” Lim said.
That’s why the association believes it’s important to think ahead of time how the healthcare system can support its frontline workers now and after the pandemic, Lim said.
One of the difficulties in the current system in Canada is that physicians are often not directly employed by the hospitals they practice in, which means emergency physicians may not have easy access to mental health resources, Lim said.
“Right now, there has been a tremendous outpouring of support from the community and a lot of counseling has been made available for free from our colleagues in mental health. This is a fantastic gesture,” Lim said. “But there is no centralized and comprehensive system for mental health support for physicians across Canada.”
While healthcare is a provincial jurisdiction, given the scope of what frontline health professionals are about to face, it would not be unreasonable to call for a national mental health support service, Lim said.
“This has been advocated by the Canadian Medical Association and it’s really, really important to safeguard the mental health of our emergency medicine staff,” Lim said. “This is not stopping the provinces from doing something similar, and I cannot stress enough how important it would be, especially after the pandemic, that we have a robust system of support for all healthcare workers on the frontline.”
‘24/7 of planning and changes’
Lim described his own experience over the last few weeks as “24/7 of planning and changes, and trying to anticipate what would be necessary in an environment that has become chaotic.”
“It’s a tremendous amount of mental effort, very little downtime and a lot of anxiety that if I don’t plan enough now, I’m going to put my healthcare worker colleagues in jeopardy,” Lim said.
“We are doing in days what used to take months, we are facing challenges that are large and massive and completely different almost on an hourly or daily basis.”
Adapting to equipment shortages and rationing

Health care workers test patients in a COVID-19 drive thru assessment centre at a Hospital in Mississauga, Ont., on Monday, March 30, 2020. (Nathan Denette/THE CANADIAN PRESS)
Because hospitals are working on a “just-in-time” supply system that is often single-sourced, the London Health Sciences Centre like many hospitals across Canada has had to carefully ration its personal protective equipment, Lim said.
“That means we’re given a certain amount of masks per shift, when we have been taught time and time again that for best practice, for patient safety that after I see a patient with a mask, that mask is thrown out and I get a fresh mask for the next patient,” Lim said.
That is no longer happening because hospitals are forced to ration their precious supply of masks in anticipation of the sheer amount of volume of patients that is expected to come in because of the pandemic, he said.
“We have to wrestle around the idea of wearing a mask that could be dirty from patient to patient,” Lim said. “These are very different circumstances than anything we have had to deal with before.”
The federal government announced Tuesday that help is on the way with Ottawa signing procurement contracts to purchase about 150 million surgical masks and 60 million N95 masks that provide better protection, as well as over 1,500 ventilators for critically ill patients.







For reasons beyond our control, and for an undetermined period of time, our comment section is now closed. However, our social networks remain open to your contributions.