Thousands of Canadians were hospitalized after deliberately harming themselves last year, according to new data from the Canadian Institute for Health Information.
The data shows that 25,000 people were admitted to hospital or died because of self-harm in 2018.
About 3,800 of them died–an average of slightly more than 10 persons a day.
Sucide is the ninth leading cause of death in Canada.

New data shows that girls and women aged 10-24, are three times more likely to be in hospital due to self-harm than males in that same age category. (Shutterstock / panitanphoto)
While the figures differ little from the previous two decades, mental health experts fear the numbers will likely rise as Canadians grapple with the effects of COVID-19, which has triggered heightened anxiety over health risks, prolonged confinement and financial insecurity.
The data–gathered before the global spread of the virus–showed that hospitalization rates were highest among girls and women aged 10-24, who were three times more likely to be in hospital due to self-harm than males in that same age category.
Death rates from suicide were highest among men 45 years and older.
People living in the lowest-income neighbourhoods had twice the rate of hospital stays (104 per 100,000 people) compared to those living in the highest-income neighbourhoods (49 per 100,000).

A candle and flowers are seen on the steps of the Alberta legislature, the spot where military veteran Ken Chan died by suicide on Dec. 2, last year. (Kim Trynacity/CBC)
Residents in rural or remote areas were also more likely to have a hospital stay for self-harm (74 per 100,000) compared with those in urban areas (63 per 100,000).
The figures don’t include people who went to emergency rooms and weren’t admitted to hospital, or those who got help from primary health-care providers, such as a family doctor, clinic or other local services.
A study released in June by the Canadian Mental Health Association found a pronounced rise in mental health concerns and suicidal thoughts, especially among subgroups that include parents, people with existing mental illness, Indigenous people and those with a disability.
It found that suicidal thoughts/feelings during the pandemic were more common for the following people:
- 1 in 5 people who already had mental illness or mental health issues (18%)
- 1 in 6 Indigenous people (16%)
- 1 in 7 with a disability (15%)
- 1 in 7 who identify as LGBTQ+ (14%)
- 1 in 10 parents of kids under 18 (9%)
CMHA chief executive officer Margaret Eaton says financial stress, isolation and fear for safety have been driving up suicidal tendencies, adding that the mental health issues will continue even as businesses and schools gradually reopen, she said.
“Now we’re seeing people having anxiety about going back to work or going back to school and wondering what that will be like for children. So that can create different emotional situations for people that can really take a toll,” Eaton told the CBC’s Kathleen Harris.
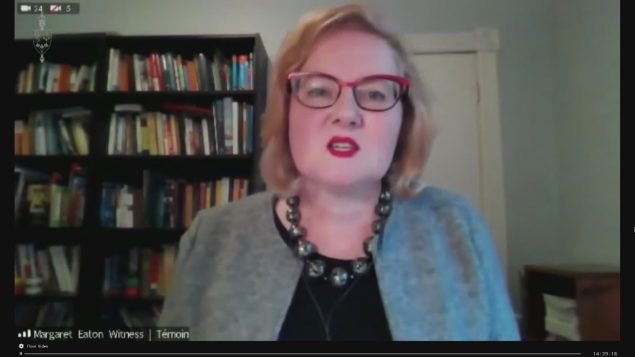
CMHA chief executive officer Margaret Eaton fears the number of people who commit suicide will increase as the the COVID-19 pandemic continues. (CBC)
“There’s real concern that there is in fact an ‘echo pandemic.’
“We’re already experiencing it and that would be once the physical health issues of COVID-19 are carrying on, we’ll also see a mental health pandemic.”
Eaton says more access to community-based services, greater efforts to lift stigma and increased government funding would help address severe mental health illnesses.
The June CMHA research found that those who were already struggling with their mental health before the pandemic are:
- twice as likely to say their mental health has declined (59% vs 33%)
- 2.5 times as likely to feel depressed (46% vs 17%)
- three times as likely to have trouble coping (28% vs 11%)
- four times as likely to have had suicidal thoughts (18% vs. 4%)
- four times as likely to have tried to harm themselves (4% vs. 1%)
In April, Eaton told Harris Canada already was failing to deliver adequate mental health services before the novel coronavirus struck and warned that officials needed to act quickly to prepare for an expected surge in demand.

Data compiled by the Canadian Institute for Health Information found that 25,000 perons were admitted to hospital or died because of self-harm in 2018. About 3,800 died. (iStock)
“We won’t know the full picture for some time but given the global reach of COVID-19, our experience tells us the mental health impacts will be significant,” she said.
The research was conducted as part of a pan-Canadian multi-year program through federal, provincial and territorial governments.
With files from Kathleen Harris of CBC News, Government of Canada







For reasons beyond our control, and for an undetermined period of time, our comment section is now closed. However, our social networks remain open to your contributions.