World leaders are meeting over the alarming global issue of antibiotic resistant bacteria. New germs are emerging that cannot be treated with drugs and if the trend continues it could lead to millions of deaths and threaten the global economy.
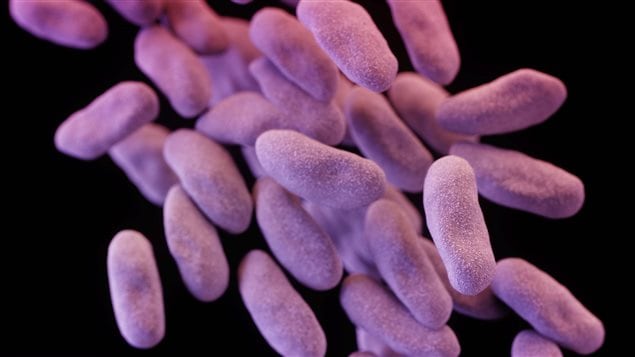
An end to current ‘medical miracles’ possible
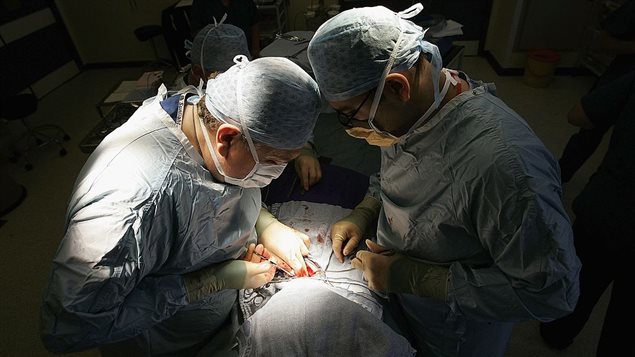
“We enjoy a lot of the miracles of modern medicine because of antibiotics,” says Lori Burrows, microbiologist and professor at McMaster University. “Think about things like caesarian sections, organ transplants, knee and hip replacements, cataract surgery, dental surgery.
“All of these things require antibiotics because you’re cutting open the skin and you’re letting bacteria in. So, you give the patient antibiotics to cover any contamination that might happen. Without them those procedures become very dangerous because you would not be able to prevent accidental infection.”
ListenSimple cuts could become lethal
What also becomes dangerous is a simple cut on the foot or anywhere on the skin, which, before antibiotics, could get infected and lead to amputation or, if infection spread, to death.

Bacteria become resistant because of overuse of antibiotics. Tons of the drugs are to treat livestock and crops, and in many developing countries they can be bought over the counter and misused.
In developed countries, patients may misuse antibiotics by not taking them for the prescribed amount of time or by sharing them with other people. Patients also sometimes demand a prescription for viral infections like the flu for which they are useless.
Drug companies not inclined develop new antibiotics
Pharmaceutical companies are not inclined to develop new antibiotics knowing they will be effective for a limited time before resistance develops. It is also more profitable for them to work on drugs for chronic conditions that must be taken over long periods of time.

‘Urgent problem’ could become uncontrollable
Burrows says there are three pillars to deal with this urgent problem “before it becomes completely uncontrollable.” The first is surveillance. Countries must track the threat—where are the resistant bacteria coming from, where are they spreading and how resistant are they.
The second is stewardship and involves training people to look after the antibiotics we have now and make sure they are not used indiscriminately.
Thinking outside the box
The third is innovation. “If we know that developing new antibiotics is only going to take us so far before resistance develops, maybe we should be thinking a little more outside the box,” suggests Burrows.
“Should we be combining antibiotics to make resistance less frequent? Should we be combining antibiotics with drugs that block resistance, which we are already starting to do?
“Can we think of non-antibiotic ways to treat disease? So, can we come up with better vaccines, can we come up with drugs that will help your immune system fight the infection on their own? These kinds of ideas have to be funded by government.”
Incurable gonorrhea on the horizon
How serious is the problem? “Very urgent,” says Burrows. “We’re starting to see strains emerge globally that are resistant to every single antibiotic that we have.”
She says common pathogens like the sexually-transmitted disease gonorrhea used to be easily treated by penicillin. It is now resistant to that drug and becoming resistant to the second line of antibiotics as well.
“You can imagine that type of disease, while (it) may not kill you immediately, it’s easily transmitted. And if it becomes completely resistant to antibiotics, that’s going to be a big problem.”






For reasons beyond our control, and for an undetermined period of time, our comment section is now closed. However, our social networks remain open to your contributions.